
Psychosis
What is Psychosis?
The word psychosis refers to a disease caused by a malfunction of the brain that disrupts contact with reality. About 3% of the population, from all causes, will suffer from some form of psychotic episode, which is a period during which they experience psychotic symptoms. Although psychosis can affect anyone (regardless of social class, education level or ethnic group), psychosis affects men slightly more than women, and the onset of the disease in men is earlier. The peak of appearance is between the ages of 15 and 35.
Most individuals with a psychotic episode will have a complete remission of their symptoms after this first episode. However, relapses are frequent: nearly 80% if treated are stop early. Like any other illness, psychosis can be treated. Thus, the adequate and regular use of antipsychotic medication, a healthy lifestyle and sleep, abstinence from drugs and moderation of alcohol consumption, as well as medical and psychosocial follow-up help to reduce this risk of relapse.
LEARN MORE
Signs and symptoms
of Psychosis
In the jargon of psychiatry, a distinction is made between positive and negative symptoms. Negative symptoms are experienced by the patient as a lack of motivation, a lack of energy, and social withdrawal. Also, the person may become very inactive or no longer interested in the things they were interested in before.
When we talk about positive symptoms, we are talking about perceptions or ideas that add to the external reality. For example, visual or auditory hallucinations and delusions are included.

One of the cardinal symptoms of psychosis is delusional thinking. These bizarre or far-fetched ideas can occur during the prodrome (period before the acute phase) or in the acute phase. When a person presents these delusions, he believes he is right, but it is still possible to change his mind by arguing and discussing.
When the intensity of the symptoms increase, the person then becomes absolutely convinced of these ideas and no argument can convince them otherwise. This is called psychosis. For example, the person may believe that people on the street are watching or trying to hurt them, or that they have supernatural powers such as telepathy. Other people may believe that aliens or the government have put a chip in their brains to control them, or that they have become the Messiah and are on a mission to convert people, or that they are possessed by spirits or suffering from a serious illness, when this is not the case.
WHO CAN HAVE PSYCHOSIS?
Psychosis can affect anyone, in any country and in any social class. A full recovery can be made if the disease is detected and treated early enough.
The disease often appears a few years earlier in men (peak onset between 15-25 years of age) than in women (peak around 25-35 years of age).
According to the most recent studies, psychosis affects slightly more men than women and is slightly more frequent in urban centres than in rural areas. Those who use cannabis at a young age are at higher risk of developing psychosis and the persistence of drug use (especially psychostimulants and cannabis) is often responsible for a bad course.
Causes of psychosis
Psychosis is a disease of the brain that leads to a loss of contact with reality. It produces an imbalance of brain neurotransmitters, particularly dopamine, which affects several cognitive spheres.
There are many causes of psychosis. For example, in some people who have a biological vulnerability (due to several genes), the addition of stressors can trigger the disease. These are biological, such as drug use (cannabis, amphetamines, cocaine) and psychosocial (financial problems, family conflicts, social isolation). The disease usually occurs in late adolescence or early adulthood when personality and coping skills are still immature, leading to difficulty in defining personal identity.
In general, the end of adolescence represents a critical stage of development during which major social and psychological changes occur: individuation in relation to the family (parental attachment gradually shifts towards relationships with peers), development of interests, skills and hobbies, discovery of intimacy and sexuality, formation and maintenance of social relationships, career choice, start of employment or higher education. The young adult focuses their mental energy on consolidating their personality and defining their life plan. When psychosis sets in, it can interrupt this process.
There are different types of psychotic disorders including psychotic bipolar illness (manic-depressive psychosis), schizophrenia, delusional disorder, substance-induced psychosis (commonly known as toxic psychosis) and others. It is the types of symptoms present, their proportion, as well as their duration and evolution over time that will determine the exact nature of each psychosis. An important factor to consider also is the individual's functioning during remission.
Although some psychotic disorders are not recurrent, most have a course with episodic manifestations, hence the need for treatment to prevent them. Rarely, sustained symptoms may require more specialized and intensive treatment.
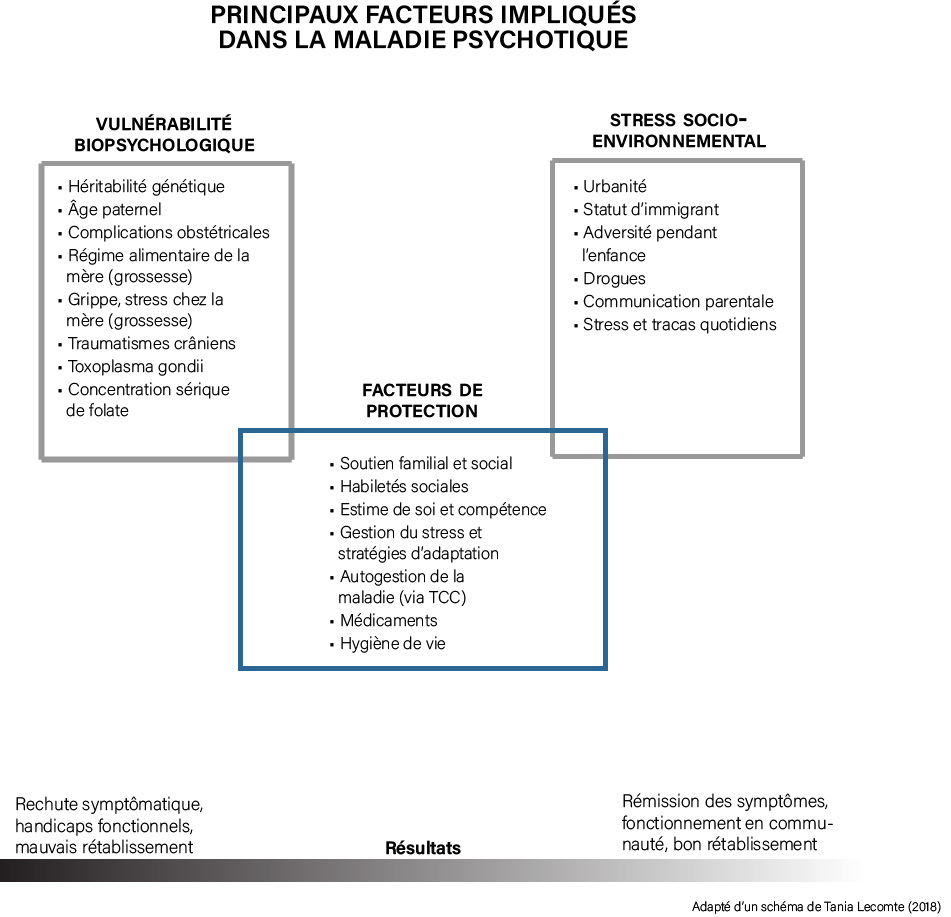
The diagram below summarizes the main factors involved in psychotic illness. The key takeaway from this diagram is that it is the sum of all these positive and negative stressors, biological and social, that determine the final state of health. So, it's important to pay attention to all of these to prevent relapse.
THE STAGES OF PSYCHOSIS
Although each psychosis presents and evolves differently, it is possible to distinguish 3 phases, or "stages", that are found in most psychoses. The duration and intensity of the phases may vary.
1. PRODROME
During the prodrome, the person shows signs of psychosis, but at a lesser intensity. During the prodrome, the person shows signs of psychosis, but to a lesser degree. This period preceding full-blown psychosis is characterized by changes in the individual's changes in the individual's thoughts, emotions, and perceptions. However, at this time, these changes are vague and difficult to detect. It may simply be a greater distrust of loved ones or bizarre or abnormal responses. During this phase, functioning, i.e. the ability to work or study, can be maintained, but more often than not, it gradually decreases. Symptoms are more often negative (isolation, withdrawal), cognitive (concentration problems, memory problems) and if there are positive symptoms (e.g. hallucinations, delirium), they are usually mild.
2. SHARP PHASE
When the individual is in the acute phase, the psychotic symptoms are clear: delusional thoughts, hallucinations and confused thinking. This person cannot be convinced that their thoughts are weird or abnormal; they firmly believe that they are right. At this point, a psychiatric evaluation, as soon as possible, as well as treatment with antipsychotic medication, are absolutely necessary for remission. In addition, in some cases, if the state of health involves a danger, it may be necessary to hospitalize the person to stabilize him/her. The duration of hospitalization is always as short as possible. In contrast to the prodromal phase, the acute individual has often become unfit for work or study, due to the positive symptoms (auditory or visual hallucinations, hearing voices, delusional thoughts) and disorganization that usually predominate. In the acute phase, it is also possible to observe symptoms at the emotional level, such as a sad mood (cries often, suicidal thoughts or suicide plans, no longer wants to eat or get out of bed) or too high (overexcited person, speaks very quickly, needs less sleep).
3. STABILIZATION
Following psychosis, the person is not immediately back on their feet and cannot necessarily return to work or school at 100% of their previous functioning. This is normal and part of the process of recovering from the disease. This is called the (partial) remission phase, i.e. the time during which the person continues to have certain symptoms at a variable intensity from one individual to another, but generally less than during the acute episode.
During this period, the risk of relapse is highest, up to 80% without medication.
Most individuals will still have negative symptoms such as social withdrawal, isolation, lack of motivation and lack of energy and cognitive disorders, such as concentration and memory problems (difficulty reading a book or watching a full movie). In some individuals, disorganization and hallucinations or delusions may persist for a longer period of time (residual phase). However, at this stage, it is quite possible to partially return to work or study, one step at a time, adjusting the medication when necessary as part of a closer follow-up during the first few months.
LEARN MORE
DRUG USE AND PSYCHOSIS
"A growing body of research shows that cannabis use, even in small amounts or occasionally, is a significant risk factor for psychosis."
CANNABIS, ALCOHOL AND OTHER DRUGS
The use of drugs and alcohol (in large quantities) decreases the effectiveness of treatment, increases vulnerability and can therefore lead to a relapse, i.e. a recurrence of psychosis symptoms. Recent studies, particularly conducted at the JAP Clinic, have shown that persistent use is associated with a poorer course in symptoms and social functioning.
Although cannabis use is widespread and commonplace, a growing body of research shows that cannabis use, even in small amounts or occasionally, is a significant risk factor for psychosis. The use of psychostimulants, such as cocaine and amphetamines (speed) as well as hallucinogens (e.g., ecstasy/MDMA), carries greater risks of psychosis and relapse than cannabis. Finally, these substances contribute to increasing the adverse effects of antipsychotics, either because their effects add up (drowsiness) or because higher doses are needed to control psychosis.
CONSUMING IS TAKING A RISK
It is sometimes difficult to convince young people to stop using, despite a first psychosis or a relapse, because it is often part of their lifestyle and it is an opportunity to socialize. Nevertheless, it is important to keep in mind that it is not because we use and do not relapse on one or more occasions that the relapse will not come. Drugs and alcohol are biological stressors for the brain and it is the cumulative stressors that leads to psychosis. Since we don't always control psychological or social stressors (job loss, breakup, etc.), using is taking a risk every time.
DID YOU KNOW?
It is well known that repeated relapses are more difficult to treat, that remission takes longer, and that they can sometimes lead to treatment-resistant psychosis, i.e., psychosis that does not respond to the various known antipsychotic drugs and often requires the addition of one or more drugs to control the acute phase.
In some cases, a stay in detoxification or reintegration therapy for mental health-substance abuse comorbidity may be necessary.
OUR MAIN PARTNERS
THE CONSEQUENCES OF PSYCHOSIS
When psychosis arises, difficulties with concentration and organization accumulate, making studying increasingly difficult. Many adolescents prefer to leave school rather than experience academic failure or feel devalued by their peers. This distances them from their main social environment, and without a place to practice, it is difficult to learn social skills. In this context, developing intimate relationships becomes extremely complex, as they are often distrustful. The illness also causes difficulties with cognition and social skills. They may see isolation as a solution to their anxiety. However, by losing their sense of identity and their bearings in the world around them, they lose a great deal of self-confidence.
When left untreated, psychosis causes a great deal of suffering and its impact has varying degrees on the person's social, family, academic and professional functioning. The "psychosocial toxicity" of the disease can have serious consequences (homelessness, job loss, deterioration of the social network, criminalization, poverty, increase in substance abuse, suicide, etc.) that can disrupt a life. However, early detection and intensive intervention can lead to a complete remission of symptoms and thus avoid prolonged suffering and disability.
